Πως αντιμετωπίζεται ένας οξύς αθλητικός τραυματισμός;
Οι τραυματισμοί των μαλακών ιστών (μύες, σύνδεσμοι και τένοντες) είναι αναπόφευκτοι στην καριέρα όλων των αθλητών. Αυτοί οι τραυματισμοί συμβαίνουν συνήθως έπειτα από χτύπημα εξωτερικού ερεθίσματος, όταν υπάρχει επαφή στο μηχανισμό της κάκωσης ή λόγω απότομης διάτασης ή/και συμπιεστίκου φορτίου στον ιστό στις περιπτώσεις όπου δεν αναφέρεται επαφή.
Οι περισσότεροι ανέπαφοι τραυματισμοί σχετίζονται με ιστούς που δέχονται απότομα υπερβολικά φορτία, έπειτα από μεγάλη περίοδο χωρίς ιδιαίτερη καταπονήση.
Τις τελευταίες δεκαετίες, η R.I.C.E.
- Rest (ξεκούραση),
- Ice (πάγος),
- Compression (συμπίεση),
- Elevation (ανύψωση σκέλους)
ήταν η κύρια θεραπευτική προσέγγιση στη διαχείριση των μυοτενόντιων και συνδεσμικών τραυματισμών, αλλά η αποτελεσματικότητά της αμφισβητείται από τους ερευνητές.
Αυτό το άρθρο παρέχει εμπλουτισμένες & επικαιροποιημένες συστάσεις για τη βέλτιστη και αποτελεσματική διαχείριση αυτών των τραυματισμών (από την φάση ξεκούρασης και ανάκαμψης έως την πρόοδο στην άσκηση και την επιστροφή σε αγωνιστική δρστηριότητα), βάσει πρόσφατης δημοσιευμένης ανασκόπησης της έρευνας.
Τι είναι απαραίτητο σε έναν οξύ τραυματισμό;
Όλοι οι ιστοί κατά το αρχικό τους στάδιο, υποβάλονται σε διαδικασία επούλωσης, η οποία είναι ζωτικής σημασίας για τη βέλτιστη ανάκαμψη και αναδιαμόρφωση του ιστού. Σύμφωνα με τα πρόσφατα δεδομένα, κατά τις πρώτες μέρες των τραυματισμών μαλακών ιστών χρειάζεται απλώς P.E.A.C.E. (ειρήνη/ηρεμία). Το ακρωνύμιο προκύπτει από τις λέξεις
- Protection (προστασία)
- Elevation (ανύψωση)
- Avoid anti-inflammatories (αποφυγή αντιφλεγμονώδους αγωγής)
- Compression (συμπίεση)
- Education (εκπαίδευση).
Η προστασία-ακινητοποίηση κατά τις πρώτες ημέρες ενός τραυματισμού είναι απαραίτητη για την ελαχιστοποίηση της αιμορραγίας και την πρόληψη υποτροπής στην τραυματισμένη περιοχή. Προστατεύστε την περιοχή περιορίζοντας τις κινήσεις που αυξάνουν τον πόνο. Η ανύψωση κατά τη διάρκεια της ανάπαυσης (τοποθέτηση του άκρου ψηλότερα από την καρδιά), βοηθάει στην αποσυμφόρηση της τραυματισμένης περιοχής.
Παρά την έλλειψη επαρκών στοιχείων, η ανύψωση θεωρείται ασφαλής μέθοδος δεδομένου του χαμηλού της ρίσκου. Αποφύγετε τα αντιφλεγμονώδη φάρμακα (NSAID’s) και τη χρήση πάγου κατά τη διάρκεια των πρώτων 48 ωρών, καθώς θα μπορούσε να διαταράξει τη διαδικασία της φλεγμονής και να οδηγήσει μακροπρόθεσμα σε ατελή επούλωση των ιστών.
Καθώς οι διάφορες φάσεις της φλεγμονής συμβάλλουν στη βέλτιστη ανάπλαση των μαλακών μορίων, δεν συνιστάται η παρεμπόδιση μιας τόσο σημαντικής διαδικασίας με τη χρήση φαρμάκων ή πάγου.
Όπου κρίνεται απαραίτητο, η δοσολογία των αντιφλεγμονωδών πρέπει πάντοτε να συνταγογραφείται από τον θεράποντα ιατρό.
Η συμπίεση (εξωτερική μηχανική πίεση) στην τραυματισμένη περιοχή, με τη χρήση περίδεσης, περιορίζει το ενδοαρθρικό οίδημα και την αιμορραγία των ιστών. Η περίδεση βελτιώνει επίσης τη λειτουργικότητα στα διαστρέμματα του αστραγάλου. Η ενημέρωση και η εκπαίδευση του ασθενούς είναι ένας σημαντικός συμβαλλόμενος παράγοντας που πρέπει πάντα να παρέχεται από ειδικό επαγγελματία υγείας, προκειμένου να δημιουργούνται ρεαλιστικές προσδοκίες στους χρόνους αποκατάστασης.
Αντί να ψάχνετε για τη “μαγική” θεραπεία στο Google, συμβουλευτείτε τον ιατρό ή τον φυσιοθεραπευτή σας για να μάθετε περισσότερα σχετικά με τη φύση του τραυματισμού, τους χρόνους αποκατάστασης και την διαχείριση των προπονητικών φορτίων.
Πόση ξεκούραση είναι απαραίτητη στον οξύ αθλητικό τραυματισμό;
Πρέπει πρώτα να ανησυχείτε για την πλήρη επούλωση και στη συνέχεια για τη διαχείριση της ανάπαυσης και της ανάκαμψης, καθώς αποτελούν βασικά συστατικά σε οποιοδήποτε προπονητικό πρόγραμμα. Εάν δεν δώσετε στο σώμα σας το χρόνο που χρειάζεται για να ανακάμψει επαρκώς και αντ ‘αυτού το ωθείτε πρώιμα στην άσκηση, ο τραυματισμός δεν θα θεραπευτεί και είναι πιθανό να μετατραπεί σε χρόνια πάθηση με επίμονα συμπτώματα.
Ο χρόνιος πόνος είναι πολύ μεγαλύτερη απειλή για τις αθλητικές σας επιδόσεις από την ανάπαυση! Γενικά είναι εφικτό να προστατεύσετε έναν τραυματισμό, διατηρώντας ταυτόχρονα τη φυσική σας κατάσταση, με τροποποιημένη άσκηση από την πρώτη μέρα.
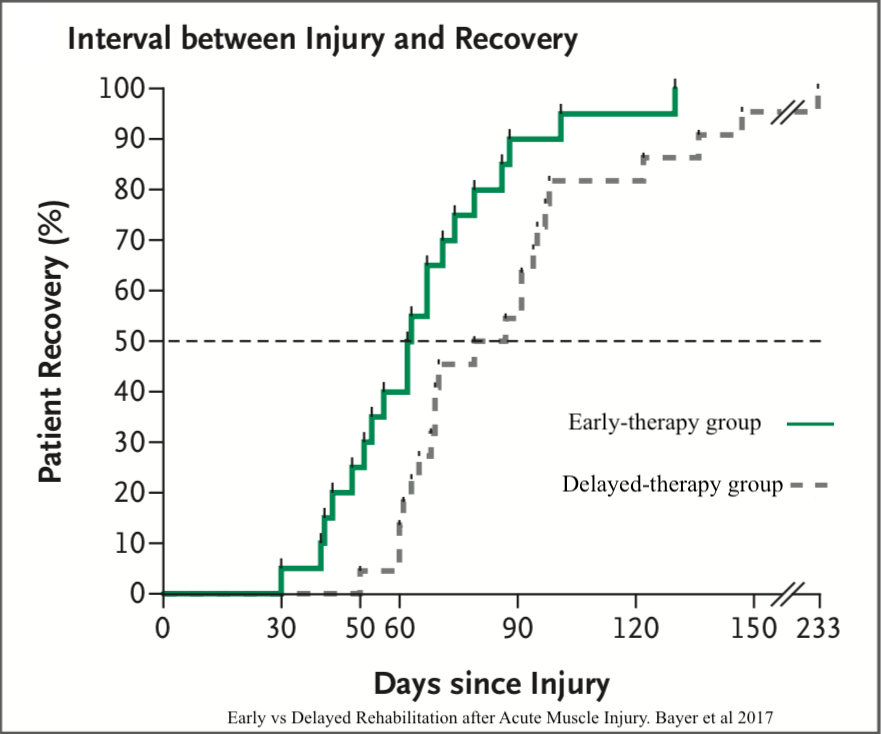
Η ξεκούραση που απαιτείται, πριν την εισαγωγή στην άσκηση, ορίζεται σε γενικές γραμμές από την συμπεριφορά του πόνου και το είδος του τραυματισμού. Οι περισσότερες ερευνητικές αναφορές θέτουν μια περίοδο ηρεμίας 48 ωρών. Σε πρόσφατη ερευνητική μελέτη, γκρουπ αθλητών με μυϊκούς τραυματισμούς που ξεκίνησαν την άσκηση νωρίτερα (2 ημέρες μετά τον τραυματισμό), μείωσαν τον χρόνο αποκατάστασης και επέστρεψαν πλήρως στην αθλητική δραστηριότητα 3 εβδομάδες νωρίτερα (κατά μέσο όρο) συγκριτικά με τους αθλητές που είχαν αναμονή 9 ημερών (βλέπε πίνακα). Δεν παρατηρήθηκε αυξημένη πιθανότητα υποτροπής του τραυματισμού μεταξύ των δύο ομάδων.
Πότε μπορώ να ξεκινήσω προπονήσεις; (φάση φόρτισης)
Όταν τα έντονα συμπτώματα υποχωρούν και δεν υπάρχει επιδείνωσή τους σε συγκεκριμένες κινήσεις, η συμπεριφορά του πόνου καθοδηγεί την σταδιακή αφαίρεση της προστασίας και την εισαγωγή της άσκησης. Σε αυτό το στάδιο, η αποκατάσταση πρέπει να χαρακτηρίζεται από διαχείριση φορτίων (Load), αισιοδοξία (Optimism), επαναγγείωση (Vascularisation) & συστηματική άσκηση (Exercise), όπου μαζί συνθέτουν το ακρωνύμιο L.O.V.E. (Αγάπη).
Η βέλτιστη διαχείριση φορτίων, κατά το στάδιο της υποξείας φάσης της αποκατάστασης, προάγει τη μακροπρόθεσμη επούλωση και αναδιαμόρφωση του ιστού, ενώ βελτιώνει την ικανότητα των τενόντων, των μυών και των συνδέσμων. Η βέλτιστη φόρτιση (optimal load) καθώς και η διαχείρηση των επίμονων συμπτωμάτων σε αθλητές, έχει περιγραφεί σε ξεχωριστό άρθρο. Η ψυχολογία του αθλητή παίζει βασικό ρόλο στην αποκατάσταση αθλητικών τραυματισμών, καθώς η συναισθηματική πίεση μπορεί να επιβραδύνει σημαντικά την επιστροφή στα επιθυμητά επίπεδα. Εϊναι απαραίτητο να υπάρχει σύμπνοια, αισιοδοξία και εμπιστοσύνη μεταξύ προπονητή, αθλητή και φυσιοθεραπευτή, για επιτυχημένη αποκατάσταση.
H αερόβια άσκηση χωρίς πόνο αποτελεί ακρογωνιαίο λίθο στη διαχείριση των μυοσκελετικών τραυματισμών, καθώς ενισχύει το κίνητρο του αθλητή ενώ παράλληλα αυξάνει τη ροή του αίματος και την αγγείωση στις τραυματισμένες δομές. Έχει επίσης επισημανθεί ότι βελτιώνει τη λειτουργικότητα, την εργασιακή απόδοση, την αισιοδοξία και μειώνει την ανάγκη για παυσίπονα. Δεν υπάρχουν σαφείς οδηγίες σχετικά με τη δοσολογία, αλλά θα πρέπει να εισάγεται το συντομότερο δυνατό. Εν τέλει, η συστηματική άσκηση αποκαταθιστά την κινητικότητα, τη δύναμη, την ελαστικότητα, την κιναισθησία και άλλες απαραίτητες πτυχές της άσκησης, για ολοκληρωμένη επιστροφή στο υψηλότερο επίπεδο.
H πρόοδος σε οποιαδήποτε δραστηριότητα καθορίζεται από τη συμπεριφορά του πόνου και το μεθοδικό σχεδιασμό.
Η οποιαδήποτε ουσιαστική εφορμογή των παραπάνω πληροφοριών, θα πρέπει να προσαρμόζεται κατάλληλα ώστε να ταιριάζει στο βιοψυχοκοινωνικό προφίλ του κάθε αθλητή.
Πηγές:










